The General Surgery Residency Program
Welcome to the General Surgery Residency Program at the Nassau University Medical Center in East Meadow, New York. We are part of NuHealth, which includes NUMC, a 530-bed tertiary care teaching facility, the A. Holly Patterson Extended Care Facility and six community Family Health Centers. The institution is home to over 20 residency and fellowship programs, training over 300 residents and fellows. Our program includes 24 active clinical residents and one research resident. We match three categorical residents and nine preliminary residents per year. Additionally, we work with multiple resident rotators from other institutions and other NUMC departments and also employ several Nurse Practitioners and Physician Assistants as part of our team.
Our program provides a robust clinical and operative experience across the various disciplines that make up General Surgery. This includes bread and butter general surgery, colorectal surgery, endoscopy, vascular and endovascular, minimally invasive surgery, bariatrics, breast, thoracic, trauma and acute care surgery. We are a Bariatric Center of Excellence. We are also an American College of Surgeons accredited Level One Trauma Center. We care for some of the most critically injured patients in Nassau County in our 11-bed Surgical and Trauma Intensive Care Unit and our six bed Surgical Post-Acute Unit, both of which are run as closed units by our Trauma/Critical Care certified faculty. Additionally, we provide off-site rotations in Cardiothoracic Surgery, Pediatric Surgery, Transplant and Surgical Oncology. We also provide NUMC rotations in Urology, Plastic Surgery, Anesthesia, Vascular and neurosurgery experience. Our residents also spend 25% of their time at our integrated site at the Long Island Jewish/Forest Hills Hospital (LIJ-FH), where they gain a significant amount of technical experience. Our chief residents graduate with approximately 950 to 1,050 cases total.
Our faculty are board certified in all of the above disciplines of general surgery and provide a broad range of patient care experiences for our residents. All of our full-time faculty actively participate in our robust academic program. Our program consists of monthly journal club, biweekly tumor board, trauma/critical care conference and mock oral examinations, weekly Morbidity & Mortality conference, Grand Rounds, basic science lectures by the faculty, textbook review and Q&A sessions. All of our residents are provided with a subscription to SCORE and TrueLearn. Our mid-level residents attend either the ATOM or ASSET course. Our chief residents are provided with SESAP and are also sent to a board review course, at no cost to them.
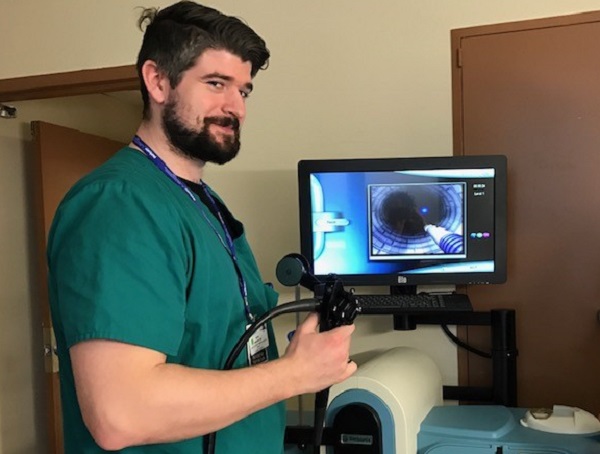
Additionally, we provide our residents with hands on skills and simulation instruction. Our skills lab includes a Simbionix (3D) Lap Mentor simulator and a GI Mentor simulator, to ensure that our residents are well-prepared for their FLS and FES examinations. We also provide Ethicon video box trainers and “white box” trainers. For our new interns, we provide an intense multi-session boot camp that includes FAST exam training, MTP instruction, suturing and knot tying sessions, VAC instruction, TLC/CT insertion, scrub/gown/glove sessions, vascular/angio orientation, ventilator instruction, SICU/SPA/Trauma room orientation, simulator instruction and mock nurse calls/sign out procedure instruction. Finally, we offer a one-year fully funded research year in Acute Care Surgery. This year is offered after the PGY-2 year. All residents who participate in the research year achieve the goal of multiple publications and some have had presentations at national meetings. Regardless of whether or not a resident does the research year, all residents are required to participate in research and to publish in peer-reviewed journals.
We recognize that the pressures of today’s residency training differ from the pressures of residency training in the past. The do-more-in-less-time work compression stress, the overwhelming burden of the current onerous electronic medical record stress, the need-to-find-time-practice-on-the-simulator stress all contribute to a new level of anxiety for residents. Recognizing this, we recently developed a “Resident Wellness Program”. We provide residents with wellness half days every quarter that they may take for things like doctor appointments, or really, any reason, no questions asked. We do dog therapy sessions several times per year. We offer periodic Tai Chi sessions (no, you don’t have to do Tai Chi, if it’s stressing you out!) and meditation/mindfulness sessions. We also have a yearly retreat that all of the residents participate in where they have a day of a fun, bonding activity, while the faculty and mid-level providers cover the patients’ needs. Some of our retreat sessions have included beach days, fishing trips, sports hub nerf wars/basketball games/obstacle courses, etc. The residents all enjoy the retreat! Join us and see what we will plan for next year!
Thank you for expressing an interest in our program. We will provide you with an outstanding clinical, academic and technical experience and hope that you will be able to join our team soon!
The surgical residency program, and Nassau University Medical Center are committed to attracting and retaining a diverse group of residents, respecting their unique identities and celebrating cultural differences. We are proud of our track record of creating a working and learning environment that is inclusive, equitable and welcoming. We welcome applications from the BIPOC and LGBTIQA+ communities.
For more information please contact Ms. Christine Barbou, Residency Program Administrator at (516) 572-3389.
Message from the Program Director:
Welcome to the Nassau University Medical Center General Surgery Residency Program! We are pleased to provide you with information about our long-standing residency program. The General Surgery training program has been accredited by the ACGME since March 1st, 1969. We have been training surgeons for over 50 years! Our department consists of a diverse group of dedicated full-time faculty who are all board certified in multiple specialties. We are devoted to the education and training of our residents, including advancing their fund of surgical knowledge, honing their technical skills and assisting them through the complexities of surgical research and publication.
The residency program consists of General Surgery, SICU and Acute Care Surgery rotations at NUMC and at our affiliate institution, Long Island Jewish Medical Center at Forest Hills. In addition, rotations in Pediatric Surgery, Surgical Oncology, Transplant and Cardiothoracic Surgery are offered at other local hospitals. These subspecialty rotations are dispersed over the PGY-2, PGY-3 and PGY-4 years. Other rotations at the home location include anesthesia, urology, vascular surgery and plastic surgery. The training culminates in the completion of the PGY-5 Chief year. Residents are given progressive amounts of hard-earned autonomy over the course of the five years. They are involved in well-supervised surgical procedures, surgical consultation and decision making processes from early on in training. The residents are strongly encouraged to follow their patients longitudinally via our clinic system from the pre-operative period, to the operative period and through their post-operative care. Demonstration of continuity of care shows ownership for one’s patients and is important in the age of duty-hour restrictions. This attention to professionalism is strongly emphasized in our program.
Residents have the opportunity to participate in a fully funded research year, sponsored by our Division of Acute Care Surgery. This outstanding opportunity gives residents a chance to explore their own areas of interest in research while remaining at the home institution at full salary. All residents who participate in the research year complete the year with multiple publications and often, with podium presentations at national meetings.
Our goal is to educate and train a diverse group of resident surgeons through state of the art educational programs that are sponsored by the major surgical governing bodies, while maintaining a nurturing environment that recognizes the humanistic needs of the trainees’ well-being. As residents progress through our program they will become skilled in providing optimal care to patients in need of surgical procedures in the areas of General Surgery, Vascular, MIS, Colorectal, Breast, Bariatric and Trauma Surgery. We also strive to provide the best possible Critical Care to the most seriously injured or ill surgical patients in Nassau County. In addition to clinical expertise, our residents learn to advance surgical knowledge through active participation in research that includes innovation and discovery, clinical application and dissemination of scholarly activity. We are extremely proud of our graduates.
Sincerely,

Elizabeth Cirincione, MD
Program Director
Program Description
The five-year Residency Program in General Surgery at NuHealth fulfills the training requirements for certification by the American Board of Surgery. It provides a graded experience, with increasing responsibility both in performance of surgical procedures and in the pre-and postoperative management of surgical patients.
The Department offers three Categorical and nine Preliminary Surgical PGY-1 positions in a comprehensive teaching program designed to prepare the candidate for further training in General Surgery or a related specialty.
There are seven full-time surgeons in the Department, which is headed by a full-time Chairman and a Vice-Chairman. The remainder of the staff includes geographic full-time, part-time, and voluntary attendings, all of whom are board-certified or board-eligible. In addition to General Surgery, the Department includes active specialty services in Trauma Surgery, Surgical Critical Care, Surgical Endoscopy, Otorhinolaryngology, Neurosurgery, Vascular Surgery, Thoracic Surgery, Bariatric Surgery, Colorectal Surgery, Urology, Surgery of the Breast, Pediatric Surgery, Head and Neck Surgery, and Hand and Plastic Surgery. The services are conducted by full-time attendings, certified in their respective specialties. All divisions and specialty sections conduct separate outpatient clinics.
The Resident Teaching Faculty is selected to ensure positive orientation towards the Department’s training goals. Residents work under close supervision with all types of clinical material to permit progressive development of surgical maturity, and are given total, supervised responsibility for the care of patients, commensurate with the individual resident’s skill and experience. Moreover, because Nassau University Medical Center is a Level I Trauma Center in the New York Emergency Medical Services System, residents gain extensive experience in the management of major trauma to round out their training, and fulfill the certification requirements in general and specialty surgery.


Curriculum Overview
FIRST POSTGRADUATE YEAR
During the initial year of the program, interns follow a strict every fourth night call schedule. They spend approximately three blocks on the General Surgery Service (GS), four blocks on the Acute Care Surgery Service (ACS), three blocks in the Surgical Intensive Care Unit (SICU) and one block each rotating on Plastic Surgery and Urology. Each rotation is 4 weeks and there are 13 four-week blocks per year. Residents get one four-week block for vacation, which can be divided over the course of the year. The General Surgery service includes all elective cases in GS and the subspecialties, except vascular. The Acute Care Surgery service includes all Trauma surgery and emergency GS and subspecialty cases. In the Intensive Care Unit, the resident is responsible for formulating and carrying out the care plan, including learning the manual and technical skills of critical care, under senior surgical resident and attending level supervision.
First-year residents are responsible for the care of all private and service patients under the supervision of the full-time and part-time teaching faculty. Bedside teaching activities and conferences are specifically organized for first-year residents and student clerks rotating through the service. House officers also participate in the management of patients in the Outpatient Department, under supervision, including discovery, formulation of treatment plans, and follow-up care for patients after discharge. During this time, the interns will also receive instruction in simulation directly from the surgical attending staff. Over the course of a two-year cycle, the formal, didactic educational program reviews the complete sphere of surgical knowledge.
SECOND POSTGRADUATE YEAR
During the second year, residents transition to senior level call schedule, which is approximately every 3.5 days or eight calls per four-week block, instead of seven. They spend one block off site at NYU Medical Center for a Transplant rotation. They also spend one block on specialty rotation at NUMC, including Gynecology, Anesthesiology or Orthopedic Surgery. All rotations provide an in-depth experience in the principles and procedural techniques of their respective disciplines.
The PGY-2 resident spends two blocks in the SICU, but this time in a supervisory role over the interns. This is an outstanding opportunity for the resident to demonstrate leadership, organizational and academic abilities. Three additional blocks are spent at our integrated affiliate, LIJ-FH, which has a full range of General, Thoracic, Vascular and Specialty Surgery. Residents do not take call at LIJ-FH but they are responsible to round every other weekend. There are also two blocks spent on vascular surgery, working directly with the vascular team in the vascular lab, endovascular suite and in the OR. There are two blocks rotating on the GS service and one block on the ACS service at NUMC. The responsibilities of the PGY-2 resident increase considerably as they transition into the consult resident role. This is an extremely important time to develop prioritization, communication and organizational skills and the all-important trust between resident and attending.
THIRD POSTGRADUATE YEAR
The PGY-3 residents spend two blocks off site. They rotate to Cohen’s Children’s Medical Center for a Pediatric Surgery rotation and also to North Shore University Hospital for a Cardiothoracic Surgery rotation. They spend one additional block on the vascular surgery service, honing previously acquired skills. They rotate to the SICU for one block, again in a supervisory role, taking no call but overseeing the interns and the PGY-2 resident. They spend three more blocks at LIJ-FH. The remaining blocks are
divided between the GS and ACS services at NUMC. During the PGY-3 year, residents will begin running traumas independently and will assume an increased measure of responsibility for direct patient care, commensurate with demonstrated capabilities and expertise. Residents also achieve a higher level of participation in OR cases and begin to supervise junior residents in the OR, under faculty guidance.
FOURTH POSTGRADUATE YEAR
The exposure to clinical surgery is intensified in the final two years of training. Residents are assigned to three more blocks at LIJ-FH, with a significant increase in OR responsibilities. They spend three additional blocks on the ACS service, honing their clinical skills and diagnostic abilities in the sickest, most severely injured patients. They also rotate to Memorial Sloan Kettering for a Surgical Oncology rotation on the pancreatic/hepatobiliary service. On the five blocks on the GS service, residents at this level are responsible for supervision of preoperative workups and the preparation of patients for operation. Under the guidance of experienced attendings, there is opportunity to exercise independent judgment and to acquire the skills necessary to serve as Chief Resident. As part of their teaching responsibility, Senior Residents actively participate in the educational programs for third-year medical students and PA students who participate in clerkships in the Department. PGY-4 residents function as chief residents whenever the chief is unavailable, including all post-call days.
FIFTH POSTGRADUATE YEAR
The Chief Resident spends four blocks each on the GS, ACS and LIJ-FH services. The chief is in charge of all patients, on his or her service and, with the advice of the teaching faculty, independently decides on treatment plans and operates on all patients or assigns less complex problems to junior residents for operation. Chief Residents are responsible for, and supervise the care of, all of the patients on their respective services, and they conduct their service’s weekly Outpatient Care Clinics, where postoperative patients are followed up on, and preoperative patients are worked up and scheduled for operation. During this final year, which is devoted entirely to clinical surgery, the residents perform major abdominal, vascular, head and neck, thoracic and pediatric procedures. They are responsible for conducting bedside rounds, and for supervision of the junior residents in the operating room, as well as for responding to requests for consultation from other services, and directing and participating in the medical student teaching program.
RESEARCH YEAR
We offer an on-site research position that is sponsored by the Division of Acute Care Surgery. This position is fully funded at the PGY-2 level salary. It allows the resident to work exclusively on research while remaining securely at the home institution. The majority of the projects are related to Acute Care Surgery, Trauma Surgery and Surgical Critical Care. However, the resident is encouraged to pursue other areas of interest with our other faculty. The position is filled by one categorical resident per year, between the PGY-2 and PGY-3 years and is highly competitive. Our residents have published their work produced during this year extensively and several have presented at national meetings, including the American College of Surgeons Clinical Congress, the Eastern Association for the Surgery of Trauma meeting and the Southwest Trauma & Acute Care Symposium.
Skills and Simulation Lab:
The department possess a skills and simulation lab that is available for resident use 24 hours per day, seven days per week. The lab includes a state of the art 3D Simbionix Lap Mentor Laparoscopic simulator and a 3D Simbionix GI Mentor Endoscopic simulator. Both simulators are equipped with all of the modules that you will require to perfect your skills prior to taking and passing the Fundamentals of Laparoscopic Surgery and Fundamentals of Endoscopic Surgery examinations. Additionally, the lab contains “white box” trainers and Ethicon video monitor laparoscopic training systems. There is also a suturing and knot tying training area where residents can practice performing basic and more advanced suturing techniques. The lab is equipped with several Ethicon suture/knot tying trays and several suture/knot tying kits for residents to practice on different materials using different sutures.
WELLNESS PROGRAM
At NUMC resident wellness is strongly emphasized. We take several steps to ensure that our residents are happy and healthy, both physically and emotionally. We offer our residents “wellness days” every quarter to allow them to take care of personal issues, no questions asked. Many times these days are used for doctor’s or dentist’s appointments, home improvement projects, car repair or even just personal family time. The reason for the request of wellness day is never required. We also provide dog therapy sessions a few times per year. Dogs have an amazing ability to create calm and ease anxiety. Bringing in therapy dogs allows the residents to unwind, relax and separate themselves from the daily stress of residency. We also offer intermittent Tai Chi classes, which the residents may choose to participate in. Finally, we offer a resident retreat every year which includes an educational/wellness session followed by a day of fun! Some of our previous retreats have focused on Positive Psychology, Resilience in Residency and Mindfulness, where they were taught meditation techniques that they can do while at work to ease anxiety. The fun portion of the day has included beach volleyball, fishing, water parks and aerial rope climbing/zip lining. The residents have an opportunity to spend quality time together outside the hospital. It’s a great bonding experience and facilitates the development of lifelong friendships.
Surgical Residency Program Interview Criteria:
Applications for one of our three categorical positions are required by November 1st of each academic year and must be submitted through ERAS. We offer three categorical interview sessions per season, in November, December and January. Each interview session is preceded by a welcome reception the night before. Details are provided upon acceptance of interview offer.
Interview requirements include (but are not limited to) the following:
- Completed application through ERAS
- Graduation from an LCME or AOA accredited program within past 5 years
- Medical Student Performance Evaluation
- Medical School Transcript
- USMLE scores (Step 1 >230/Pass; Step 2 > 240)
- Equivalent COMLEX scores
- Three letters of recommendation
- Letter of recommendation from Program Director if in a preliminary position
- US citizen/Permanent Resident/J-1 visa only
- Valid ECFMG certificate
- Clinical experience in a US teaching hospital
- Publications strongly encouraged
The Program Director, Chairman, and members of the Interview Committee review the applications and select the candidates they believe to be the most qualified for the available positions within our training program. After visiting the department and being interviewed by the faculty, candidates for ranking are selected based on their academic credentials, extra-curricular activities, communication skills, personal qualities (i.e. integrity, motivation) and their overall “fit” with our team. At the discretion of the Interview Committee, social media websites may be screened prior to ranking a candidate.
We look forward to having an opportunity to review your application and meet you! Please contact our Residency Program Administrator, Ms. Christine Barbou, at (516) 572-3389 if you need any additional information. Thank you for your interest in our program.

Christine Barbou, MA, Surgical Residency Program Administrator
Christine joined the Department of Surgery in 2013. She has a degree in English as well as a Master’s Degree in Elementary Education. She is responsible for the organization and implementation of all residency program administrative needs.
Fellowship Matches:
2020 Graduates:
- Minimally Invasive Surgery: Kaiser Permanente, Sacramento, CA
- Plastic Surgery: Tulane University, New Orleans, LA
- General Surgery Faculty Practice, Batesville, AR
2019 Graduates:
- Plastic Surgery: University of Alabama, Birmingham, AL
- General Surgery Private Practice, Suffolk County, NY
- Critical Care: Cooper University Health Care, Camden, NJ
2018 Graduates:
- Breast Oncology: Beth Israel/St.Luke’s Hospital, New York, NY
- Vascular Surgery: Michigan State University, Flint, MI
- Burn Surgery: The Johns Hopkins Hospital, Baltimore, MD; followed by
- Plastic Surgery at Florida State University, Tallahassee, FL
2017 Graduates:
- Plastic Surgery: NUMC, East Meadow, NY
- Breast Oncology: Georgetown, Washington DC
- General Surgery Faculty Practice, Westchester County, NY
2016 Graduates:
- Breast Oncology: John Wayne Cancer Institute, Santa Monica, CA
- Endocrine Surgery: Calgary University Medical Center, Calgary, AB, Canada
- General Surgery Faculty Practice, Flint, MI
2015 Graduates:
- Trauma/Critical Care: Stroger Hospital of Cook County, Chicago, IL
- Trauma/Critical Care: Stroger Hospital of Cook County, Chicago, IL
- Trauma/Critical Care: Parkland Hospital, Dallas TX
2014 Graduates:
- Minimally Invasive Surgery: Westchester County Medical Center, Valhalla, NY
- Minimally Invasive Surgery: University of Texas HSC, Houston, TX
- Trauma/Critical Care: Stroger Hospital of Cook County, Chicago, IL
2013 Graduates:
- Plastic Surgery: Temple University Hospital, Philadelphia, PA
- Minimally Invasive Surgery: Albany Medical Center, Albany, NY
- Trauma/Critical Care: University of California, Irvine, CA
2012 Graduates:
- Head & Neck surgery: The Johns Hopkins Hospital, Baltimore, MD
- Colorectal Surgery: Louisiana State University, Shreveport, LA
- Plastic Surgery: University of Alabama, Birmingham, AL
2011 Graduates:
- Vascular Surgery: Englewood Hospital, Englewood, NJ
- Colorectal Surgery: St. Vincent’s Hospital, Erie, PA
- Surgical Critical Care: The Johns Hopkins Hospital, Baltimore, MD
2010 graduates:
- Surgical Oncology: Virginia Commonwealth University Medical Center, Richmond, VA
- Vascular Surgery: Staten Island University Hospital, Staten Island, NY
- General Surgery Private Practice, Suffolk County, NY
A few comments from our residents:
- “The camaraderie among us residents is incredible. We stand with and for each other. We always put our patients first collectively and if any one of us are in need of anything, professionally or personally, there is never any hesitation among us to assist each other in whichever way we can. We celebrate each other’s life events, have impromptu gatherings and take a personal interest to teach each other. Simply put, we are a family.”
- “The academic program at NUMC provides us with ample opportunities to grow academically and professionally. There is protected academic time along with the opportunity to join many faculty on current research projects.”
- “The research year is one of the greatest opportunities, one of which I was able to take advantage of. It has brought me tremendous amount of success that was encouraged by the faculty here at NUMC.”
- “Our attendings take a personal interest in each of our successes and failures. They are there to commend your accomplishments as well as aid you on your deficiencies. I have no doubt that pursuing a fellowship, going directly into practice or pursuing an academic career are equally tenable options for me after NUMC.”
- “Surgery residency requires an innate quality of resilience, perseverance and self-discipline. With those qualities and the opportunity to train here at NUMC, you will become a successful, safe and skilled clinical and academic surgeon.”
- “The last few years have been filled with challenges (both mentally and emotionally), heartache (in particular, when caring for a critical patient who will not seem to turn the corner), and great reward. This reward comes in the form of great friendships made with fellow residents and mentors, vast surgical knowledge gained through our structured academic curriculum, and the newfound confidence that I can take care of the whole surgical patient from admission through the operating room and to discharge.”
- “NUMC gave me the opportunity to see and treat a vast spectrum of surgical disease. I am proud to tell people I train at NUMC because the program builds a strong, smart, and capable surgeon from the ground up.”
- “The attending surgeons are fully invested in the residents as if they were raising their own children, they enjoy watching our growth mentally and technically. NUMC is a great place to train to become a skilled, confident and most importantly a safe surgeon.”
- “What is life like as a NUMC surgical resident? A few words quickly come to mind – fast paced, autonomous and challenging….”
- “The teaching environment which is fostered in the program is carried throughout the surgical floor, OR, ICU and outside rotations. Such an environment promotes the education of both the art and science of surgery, while supporting residents’ academic pursuits and our professional development.”
- “We have a strong camaraderie amongst the residents as well as with the faculty and other staff. Many of us establish life-long friendships, and the strength of our friendships ultimately leads to the creation of a strong team.”
- “While you may choose to apply for a fellowship at the end of that five years, surgical residents from NUMC are well-equipped and adequately prepared to enter the workforce as a general surgeon where patients will put their lives, in literally, your hands. That’s something this program and the Attending’s’ take very seriously.”